Best Sweeteners for Diabetics
 Preventable But On The Rise
Preventable But On The Rise
Rising rates of diabetes have made this chronic disease a part of everyday discourse. Despite growing appreciation for the importance of this problem, the real gist of what drives the development of diabetes remains somewhat mysterious. A deeper understanding of these issues is vital to adopting dietary measures that can help prevent and treat diabetes. Central to diabetes management is appropriate blood glucose levels, a feat made more feasible (and delicious!) with the use of alternative sweeteners. Choosing the best sweeteners for diabetics becomes clear after first exploring the mechanisms that work to help and hinder blood sugar levels.
Why We Crave the White Stuff: The Energetic Demand for Simple Sugars
 The brain is the single most energy-demanding organ of the body and its primary fuel is the simple sugar glucose. For this reason, blood sugar levels are tightly regulated by the body in order to remain within an optimal range for brain function. While some other cells of the body also thrive on glucose, most require the presence of insulin for this sugar to flow into the cells.
The brain is the single most energy-demanding organ of the body and its primary fuel is the simple sugar glucose. For this reason, blood sugar levels are tightly regulated by the body in order to remain within an optimal range for brain function. While some other cells of the body also thrive on glucose, most require the presence of insulin for this sugar to flow into the cells.
At meal time, blood sugar levels begin to rise according to the amount and type of food eaten. Sensing this rise, the pancreas releases insulin, a hormone that allows cells to absorb the sugar present in the blood. The ability of insulin to do its job is dependent on special insulin receptors located on the surface of cells. They act as a lock accessible only to the insulin key. The speed with which the cells are able to accommodate a given amount of glucose is characteristic of how well this lock and key system is functioning as a whole.
Too Much of a Good Thing: Losing Control and Developing Diabetes
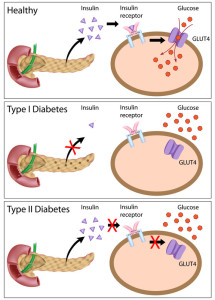 There are a number of reasons why diabetes can develop but they all share a common denominator: insufficient insulin activity. This may be due to a malfunction in either part of the insulin and receptor lock and key system but generally appears as two clinical entities referred to as Type 1 and Type 2 diabetes.
There are a number of reasons why diabetes can develop but they all share a common denominator: insufficient insulin activity. This may be due to a malfunction in either part of the insulin and receptor lock and key system but generally appears as two clinical entities referred to as Type 1 and Type 2 diabetes.
For one reason or another, the pancreas of some people wears out early in life and they develop what is commonly known as juvenile-onset or Type 1 diabetes. With no natural insulin production, people with Type 1 diabetes require an external source of insulin from the outset of the disease, making them “insulin-dependent.”
The most common form of the disease, Type 2 diabetes, is linked to obesity and excessive sugar intake essentially wearing-out the body’s ability to produce enough insulin. Type 2 begins as an “insulin-independent” state wherein dietary measures are the primary determinant for the development of symptoms. Continuously elevated blood sugar levels demand more insulin from the pancreas, causing a fatigue that can eventually halt natural insulin production all together. As a result, Type 2 diabetics can become insulin-dependent.
It gets worse. The impending development of Type 2 diabetes is also often signaled by a state of insulin-resistance. Long term excess sugar intake causes over-stimulation of insulin receptors, making them less-sensitive to the effects of the hormone. Even though the body still produces normal levels of insulin, this is no longer a sufficient quantity to open the door of the cells to let in the sugar once insulin-resistance has developed.
Given the tendency for this form to develop later in life, Type 2 is also known as adult-onset diabetes, however the disease can now be found in an ever-growing number of school children. This may be due in part to increasing rates of obesity, a leading risk factor for the development of Type 2 diabetes.
Whether from too little hormone or increasingly sluggish receptors, the overall result underlying any case of diabetes is insufficient insulin activity.
Regaining Control: Key Attributes of Sweeteners for Diabetics
 The good news is that a combination of regular medical supervision and good dietary measures can help reestablish healthy blood sugar levels. A very useful tool for designing a diabetic diet is the glycemic index. This value describes the amount and rate of insulin release stimulated by a given food. Glucose has a glycemic index, or “GI,” of 100 and table sugar, a combination of glucose and fructose, has a GI of 65. Although fructose, the form of simple sugar commonly found in fruit, has a GI of only 25, the amount of fructose in the diet should be minimized. The metabolism of fructose to glucose takes a heavy toll on the liver, which remains associated with an increased risk of obesity. Just as the high fructose corn syrup in sodas is a bad option for health, so too is excess fructose consumption from any source, including fruit.
The good news is that a combination of regular medical supervision and good dietary measures can help reestablish healthy blood sugar levels. A very useful tool for designing a diabetic diet is the glycemic index. This value describes the amount and rate of insulin release stimulated by a given food. Glucose has a glycemic index, or “GI,” of 100 and table sugar, a combination of glucose and fructose, has a GI of 65. Although fructose, the form of simple sugar commonly found in fruit, has a GI of only 25, the amount of fructose in the diet should be minimized. The metabolism of fructose to glucose takes a heavy toll on the liver, which remains associated with an increased risk of obesity. Just as the high fructose corn syrup in sodas is a bad option for health, so too is excess fructose consumption from any source, including fruit.
While a number of low and zero GI artificial sweeteners are available, the safety and long-term effects of these products remains unclear. A number of health problems including cancers, immune dysfunction, neurological disorders and chronic diseases of all sorts are suspected of being related to the regular consumption of certain artificial sweeteners. Nearly as distressing are the studies showing that these products, which were developed as weight loss aides, are associated with weight gain! Fortunately, a number of natural sweeteners have become widely available, several of which have a favorable glycemic profile.
Sweet Possibilities: The Leading Sugar Substitutes for Healthy Blood Sugar Management
Sugar Alcohols such as sorbitol, xylitol and erythritol can be an appealing alternative to artificial sweeteners. These no calorie, zero GI options are already used in a number of processed foods. However, many consumers are distressed by the digestive discomfort, bloating and diarrhea commonly associated with their use. Erythritol is reported to have the lowest rates of digestive side effects and may be found at a few specialty shops in granulated form.
Stevia is one of several plant-derived natural sweeteners and has been recommended by diabetes experts because it has a GI of 0. A blend of non-sugar steviol glycosides gives the stevia plant a super sweet taste however the commercially available derivatives contain only one steviol glycoside, rebaudioside A. Many consumers are concerned about the chemicals used in manufacturing this compound and the unknown effects from its isolated consumption. Although the whole food has been used for centuries, intake of this single component in increased quantities may effect the body in as of yet unappreciated ways.
Agave syrup is a low glycemic food that is available in a relatively unprocessed format. Unfortunately, its GI of only 15 is attributable to its high content of fructose. As a result, the liver and waist-line may still pay a high price for this low GI sugar substitute.
Coconut palm sugar is a natural sweetener with a GI of 35 and a very low fraction of fructose. Minimal processing allows it to retain nutritional qualities such as vitamins, minerals and amino acids. Concerns, however, have been raised that its precise nutritional profile varies too substantially according to region and season.
 Yacon syrup, derived from the tuberous Smallanthus sonchifolius plant native to South America, has been used for centuries as a sweetener, food source and diabetes treatment. With a sweet taste attributable to the fructans FOS (fructooligosaccharides) and inulin, this low glycemic food has a GI of only 1. FOS and inulin provide the additional benefit of functioning as prebiotics, providing support for a healthy balance of intestinal flora and gently promoting overall digestive health.
Yacon syrup, derived from the tuberous Smallanthus sonchifolius plant native to South America, has been used for centuries as a sweetener, food source and diabetes treatment. With a sweet taste attributable to the fructans FOS (fructooligosaccharides) and inulin, this low glycemic food has a GI of only 1. FOS and inulin provide the additional benefit of functioning as prebiotics, providing support for a healthy balance of intestinal flora and gently promoting overall digestive health.
Yacon syrup is also rich in vitamins, minerals and antioxidants. Recently, it has become the focus of numerous studies showing a beneficial effect on blood sugar values as well as weight loss. This makes Yacon syrup a time-tested, clinically verified, sweetly delicious source of multiple health-promoting components. Whether used alone as a dietary supplement or in recipes and drinks, Yacon syrup supports proper blood sugar regulation and overall well being making it a clear leader among natural sweeteners and the best sugar substitute.
Click Here To Buy Yacon Syrup Gold on Amazon
If you’ve enjoyed this article, please link back to us at:
[https://goldsourcelabs.com/?p=904]

Leave a Reply